Harmony Health Group Accepts BCBS Insurance Coverage
Suboxone has transformed the landscape of addiction treatment for those who are struggling with opioid use disorder by reducing cravings and withdrawal symptoms, allowing them to address the root of their addiction through various behavioral treatment approaches. By providing relief from physical and psychological symptoms common in addiction, Suboxone can help you reclaim control of your life.
Check Your BCBS Suboxone Treatment Coverage Levels with Harmony Health Group
You can check your insurance coverage levels by calling us on: (866) 461-4474
Who is Blue Cross Blue Shield (BCBS) Health Insurance Provider?
BlueCross Blue Shield’s history can be traced back to the 1920s, when it was developed in Texas to help teachers who were struggling to afford treatment for their medical needs. When it began, BCBS provided pre-paid hospital plans that allowed teachers to access hospital care for a small fee, known as “Blue Cross”.
A decade later, employers in California wanted a similar program to help with their medical needs, so they developed “Blue Shield”, which provided pre-paid services for employees. These programs grew in popularity and eventually merged in 1972, forming the Blue Cross Blue Shield organization. When this merger occurred, members were able to receive standardized care that maintained their local autonomy. Fast-forward to the present day, BlueCross Blue Shield is one of the leading health insurance providers with plans providing coverage for millions of families, individuals, and businesses. BCBS has high standards for comprehensive and high-quality healthcare coverage for its members to promote their overall health and wellness.
Some of BCBS Healthcare Brands, Products & Services
Understanding What is Suboxone Medication Treatment?
Suboxone treatment is a form of medication-assisted treatment that utilizes medication in addition to addiction treatment services. Suboxone has two ingredients; buprenorphine and naloxone, which can decrease cravings and withdrawal associated with opioid use disorder (OUD) and reduce the risk of an overdose if you were to continue using, relapse, or abuse your medication.
Suboxone treatment can begin at the beginning stages of recovery in a detoxification program, and continue to support you as you progress through your recovery if necessary. Addiction treatment programs utilize evidence-based treatment approaches that provide you with comprehensive care, allowing you to get to the root of your addiction and move forward in your recovery. Different treatment programs are intended for individuals with varying symptoms and concerns, which means that the level of care you need will be dependent on personal characteristics including the severity of your addiction, your level of functioning, the presence of physical health concerns, and if you are living with any other mental health concerns. The Harmony Health Group is a leading addiction treatment provider on the East Coast with several Blue Cross Blue Shield Suboxone rehab centers that can walk beside you as you navigate your recovery. We invite you to contact us today by dialing (866) 474-4474.
How Does Suboxone Work to Treat Addiction from Substances?
The two ingredients in Suboxone have their unique purposes and functions. Buprenorphine is a partial opioid agonist, that can alleviate symptoms associated with withdrawal including nausea, vomiting, sweating, muscle aches, and insomnia. Naloxone is an opioid antagonist, that blocks the effects of opioids, which can reduce the risk of misuse. Suboxone can be an effective medication option for individuals who follow their medication regimen and are actively working on establishing their recovery with the use of healthy coping and relapse-prevention skills.
National Statistics on Addictions and Suboxone Treatment
Does Blue Cross Blue Shield Cover Suboxone Addiction Treatment?
Yes, Blue Cross Blue Shield (BCBS) does cover Suboxone treatment, offering a lifeline to those grappling with opioid use disorder. This coverage plays a pivotal role in supporting individuals on their path to recovery by providing access to medication-assisted treatment (MAT). Suboxone, a preferred medication under many BCBS plans, is recognized for its effectiveness in reducing cravings and withdrawal symptoms associated with opioid addiction. Coverage can include various forms of Suboxone treatment, from initial consultations with Suboxone doctors that take Blue Cross Blue Shield to ongoing medication management. It’s important to note, however, that coverage levels for Suboxone treatment can vary widely, depending on the specifics of your BCBS plan, the healthcare provider, and the treatment protocol recommended.
Navigating the complexities of insurance coverage for Suboxone treatment can feel daunting, but you’re not alone. Harmony Recovery Group is here to help you understand your BCBS Suboxone coverage and explore your treatment options. Our compassionate team believes in empowering you with the knowledge and support needed to make informed decisions about your recovery journey. By reaching out to us, you’ll find a supportive ally ready to assist you in uncovering the details of your insurance benefits for Suboxone treatment. Let Harmony Recovery Group be your guide in accessing the care you need, ensuring that you feel supported every step of the way towards a healthier, substance-free life.
Does BCBS Cover Suboxone Medication, Doctors, and Clinics for Addiction?
Yes, Blue Cross Blue Shield (BCBS) does cover Suboxone medication, suboxone doctors, and suboxone clinics, providing essential support for individuals seeking treatment for opioid use disorder. This coverage is a critical component of the journey towards recovery, offering hope and practical assistance to those in need. BCBS policies typically encompass a range of Suboxone treatment types, including outpatient visits to Suboxone clinics near you, consultations with Suboxone doctors accepting new patients, and even walk-in Suboxone centers for immediate support. Additionally, for those managing both addiction and pain, Suboxone and certain pain medications may also be covered, reflecting BCBS’s comprehensive approach to opioid use disorder treatment. However, it’s important to understand that coverage levels and the specifics of what is covered can vary widely depending on your particular BCBS plan, the state you reside in, and the healthcare provider’s network status.
If you’re navigating the complexities of finding a Suboxone clinic or doctor near you that accepts BCBS, Harmony Recovery Group is here to help. We understand how overwhelming it can feel trying to understand the specifics of your insurance coverage while seeking the best possible care for yourself or a loved one. Our team is dedicated to providing compassionate, supportive, and empowering guidance to help you make informed decisions about your Suboxone treatment options. By reaching out to Harmony Recovery Group, you’ll gain clarity on your BCBS coverage levels for Suboxone treatment, ensuring that you can access the necessary care without undue stress. Let us assist you in taking this crucial step towards recovery, offering a beacon of hope and the promise of a healthier future.
What Does Blue Cross Blue Shield (BCBS) Cover for Suboxone Rehab Treatment?
Coverage often extends to a variety of settings, including visits to Suboxone clinics near you and consultations with Suboxone doctors that take Blue Cross Blue Shield. While BCBS considers Suboxone a preferred medication for treating substance abuse, indicating no need for prior authorization in many cases, it’s essential to understand that coverage specifics, such as the type of Suboxone medication (brand name vs. generic) and treatment duration, can vary. This variability underscores the importance of familiarizing yourself with your plan’s details to ensure you can fully leverage your benefits.
Suboxone can be used on a short-term or long-term basis, depending on the needs of the individual. In detoxification programs, Suboxone can be used to decrease the distress associated with withdrawal symptoms, whereas later in recovery it can be used to decrease cravings and support individuals in their recovery. Blue Cross Blue Shield coverage may vary based on the details of your plan, which is why we encourage you to verify your insurance and familiarize yourself with the details of your plan.
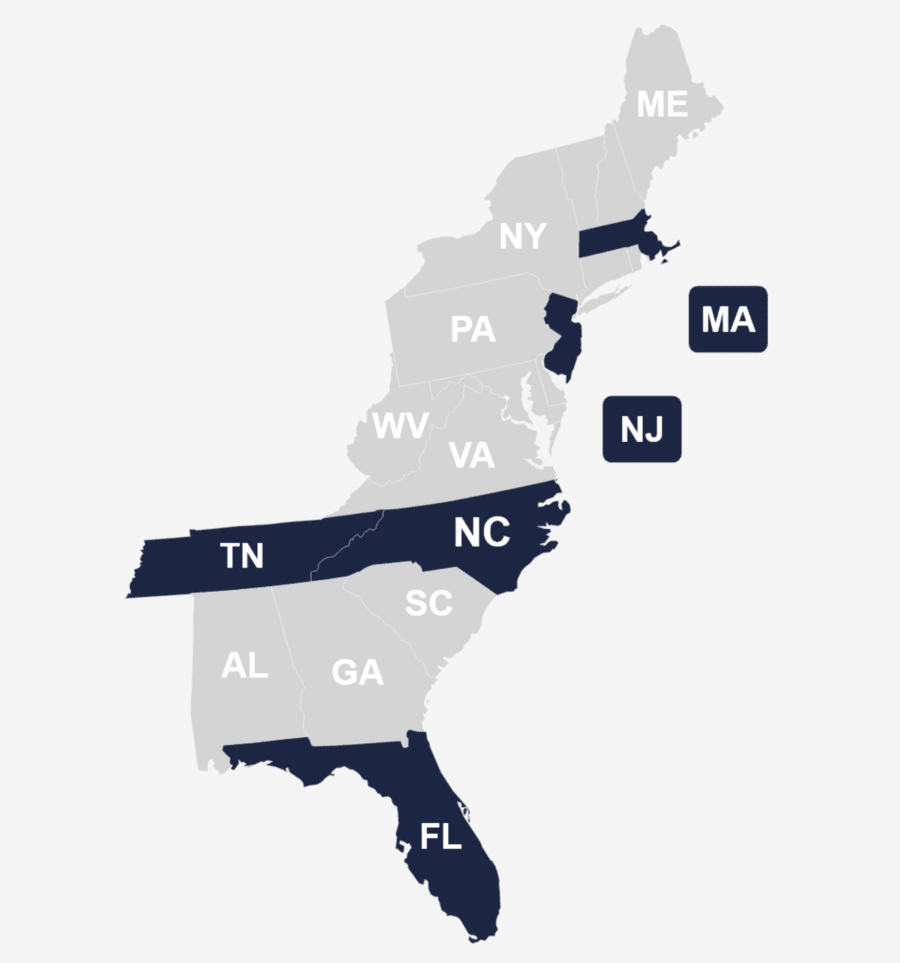
Suboxone Treatment Centers That Take Blue Cross Blue Shield
As a leading substance abuse and mental health treatment provider, the Harmony Drug and Alcohol Addiction Recovery Group has ten treatment facilities located across the East Coast. Our treatment facilities accept several major health insurance companies, including Blue Cross Blue Shield. Our Admission Counselors are available now to verify your insurance and guide you through the admission process!
Suboxone Treatment Provider in Massachusetts
Suboxone Treatment Provider in Tennessee
Suboxone Treatment Provider in New Jersey
Suboxone Treatment Provider in North Carolina
Suboxone Treatment Provider in Florida
Harmony offers a multitude of locations up and down the East Coast for behavioral health services. Call us to learn about our facilities and treatment options.
Does Blue Cross Blue Shield (BCBS) Cover Suboxone Abuse Therapy & Counseling?
Finding a BCBS doctor that prescribes Suboxone medication can feel like a daunting task, especially when you’re already navigating the complexities of recovery. The journey towards healing requires not just medical treatment but also a supportive and understanding environment that fosters growth and resilience. At Harmony Healing Group, we recognize the importance of matching you with care providers who not only have the expertise in addiction treatment but also deeply understand the challenges you’re facing. By reaching out to us, you can discuss your treatment needs and insurance coverage in a compassionate and non-judgmental setting. Our team is equipped with doctors who are experienced in prescribing Suboxone, all within a framework that honors your individual journey and respects the courage it takes to seek help.
Embarking on this path with Harmony Healing Group means you’re not alone in deciphering the intricacies of your BCBS coverage for Suboxone treatment. We’re here to empower you with information and support, ensuring that your treatment plan aligns with both your recovery goals and insurance benefits. Our commitment to providing empathetic, comprehensive care reflects our belief in the promise of recovery for every individual struggling with mental health issues. Let us be your partner in navigating the process, offering reassurance and guidance every step of the way towards a healthier, more fulfilling life.
Do Suboxone Doctors Accept BCBS Health Insurance Coverage?
Yes, doctors who prescribe Suboxone to treat opioid use disorders often accept health insurance, including BCBS. Your healthcare plan may require that you obtain a pre-authorization or a referral before you begin taking your new medication. If you are unsure if this is needed for your claims to be approved, we encourage you to verify your coverage today.
HHG Contact Us
What are Benefits of Using Suboxone to Treat Opioid Use Disorder?
Yes, typically Blue Cross Blue Shield offers coverage levels for inpatient or residential substance abuse counseling and therapy. Counseling and therapy are foundational strategies for mental health and substance abuse treatment to help individuals identify triggers, develop coping strategies, and address the physical, psychological, and emotional aspects of addiction.
Does Blue Cross Blue Shield Cover Inpatient Suboxone Treatment?
Yes, typically Blue Cross Blue Shield offers coverage levels for inpatient or residential substance abuse counseling and therapy. Counseling and therapy are foundational strategies for mental health and substance abuse treatment to help individuals identify triggers, develop coping strategies, and address the physical, psychological, and emotional aspects of addiction.
Benefit: Reduces Cravings and Withdrawal Symptoms
Benefit: Prevents Overdose
Benefit: Improves Quality of Life
How Much Does Suboxone Treatment Cost Without BCBS Health Insurance?
If you find yourself wondering about the cost of Suboxone treatment programs, know that many people worry about being able to afford the treatment they need. Suboxone treatment costs vary with the dosage used, where you live, and the length of time the medication is used. On average, Suboxone treatment cost is approximately $115.00 per week or $5,980.00 annually.
If you can use healthcare insurance, you may be eligible for partial or full coverage of your substance abuse treatment, including medication-assisted treatment options. If you are interested in learning about the details of your health insurance plan, and how it would affect the cost of Suboxone treatment, we encourage you to contact the Harmony Health Center today. Our Admissions Counselors can provide you with valuable insight and guidance that can support you in your recovery journey.
How To Check Blue Cross Blue Shield Coverage Levels for Treatment?
If you are committed to taking the next step in your recovery and getting help for your use of drugs or alcohol, you may find yourself searching for “Blue Cross Blue Shield Suboxone providers near me” or “Does Blue Cross Blue Shield cover Suboxone rehab?” online. Keep in mind that your insurance plan determines your coverage for treatment.
Once you have an idea of available treatment providers in your area, you can contact them to learn about their available treatment options. Typically, BCBS provides coverage for detoxification, inpatient treatment programs, outpatient treatment, medication-assisted treatment, and dual diagnosis treatment for policyholders.
How To Get Blue Cross Blue Shield To Pay For Suboxone Treatment
Once you have verified your insurance and chosen a treatment provider, you are closer to beginning the next chapter of your recovery! Typically, after a treatment provider has verified your insurance, you can begin engaging in your treatment, which will then automatically submit a claim to BCBS for you.
While there may be necessary steps to take before you can begin engaging in treatment, once your insurance is verified, and you have the proper authorizations needed, you should not have to worry too much about your claims being processed. If you have a claim denied by your insurance provider, you can appeal with a detailed explanation about why the care you received was necessary for your health.
Related Coverage For Suboxone Treatment
Related BCBS Coverage Articles
Suboxone Treatment Statistics in the United States
- Approximately 3/4 of those prescribed Suboxone in 2019 did not misuse or abuse their prescription and followed their medication regimen
- An estimated 1.7 million individuals reported using their medication as prescribed, while 700,000 endorsed misusing their prescription
- 27.3% of those who misused their prescription said they did so “because I’m hooked”
- 20.5% of those who misused Suboxone reported that this was done in an attempt to self-medicate for withdrawal symptoms and to decrease cravings
- The rates of Suboxone misuse and abuse decreased from 2015 to 2019
- Less than 18% of those living with an OUD in 2019 utilized MAT treatment options
- The Centers for Disease Control and Prevention reported that the national buprenorphine rates increased from 2019 to 2022 with the highest rate in 2021 with over 16 million prescriptions
- States with the lowest dispensing rates in 2022 included Iowa, Texas, California, and Hawaii
- Dispensing rates for Suboxone i
- Florida: 2.9 per 100 persons
- Massachusetts: 9.6 per 100 persons
- North Carolina: 5.7 per 100 persons
- New Jersey: 3.8 per 100 persons
- Tennessee: 10.9 per 100 persons
Get in touch with Harmony Health Group to find out about our rehab admissions process, free assessment, treatment options or to check your insurance coverage levels. Your first step to recovery starts here!
Provide Your Contact Details

8520 Cliff Cameron Dr. Ste 450, Charlotte, NC 28269
